The patients themselves pay for most cosmetic procedures. This is because cosmetic procedures are for aesthetic purposes instead of medical. However, as with everything, there are some exceptions. So, what cosmetic surgery is covered by insurance?
Just because your outward appearance improves does not mean there are no medical benefits. We will explore the cosmetic surgery insurance options below, so keep reading to find out.
[ez-toc]
What Cosmetic Surgery Is Covered by Insurance?
Health insurance covers plastic surgery procedures that are medically necessary, such as reconstructive surgery. Otherwise, cosmetic procedures to enhance the aesthetic appearance are deemed elective.
Medical insurance does not cover elective cosmetic procedures whose only goal is aesthetic improvement. But before deciding to pay your plastic surgery cost out of pocket, research if there are any chances for your insurance to cover it.
Many cosmetic surgeries may fall into a gray area between medically necessary and elective. This means that depending on your insurance provider, they may cover the cost. So, cosmetic procedures that are covered by insurance may be the following:
- Breast surgery
- Butt lift
- Rhinoplasty
- Eyelid surgery
- Skin removal
- Botox
However, it’s important to note that insurance coverage for cosmetic surgery can vary based on individual insurance plans and policies.
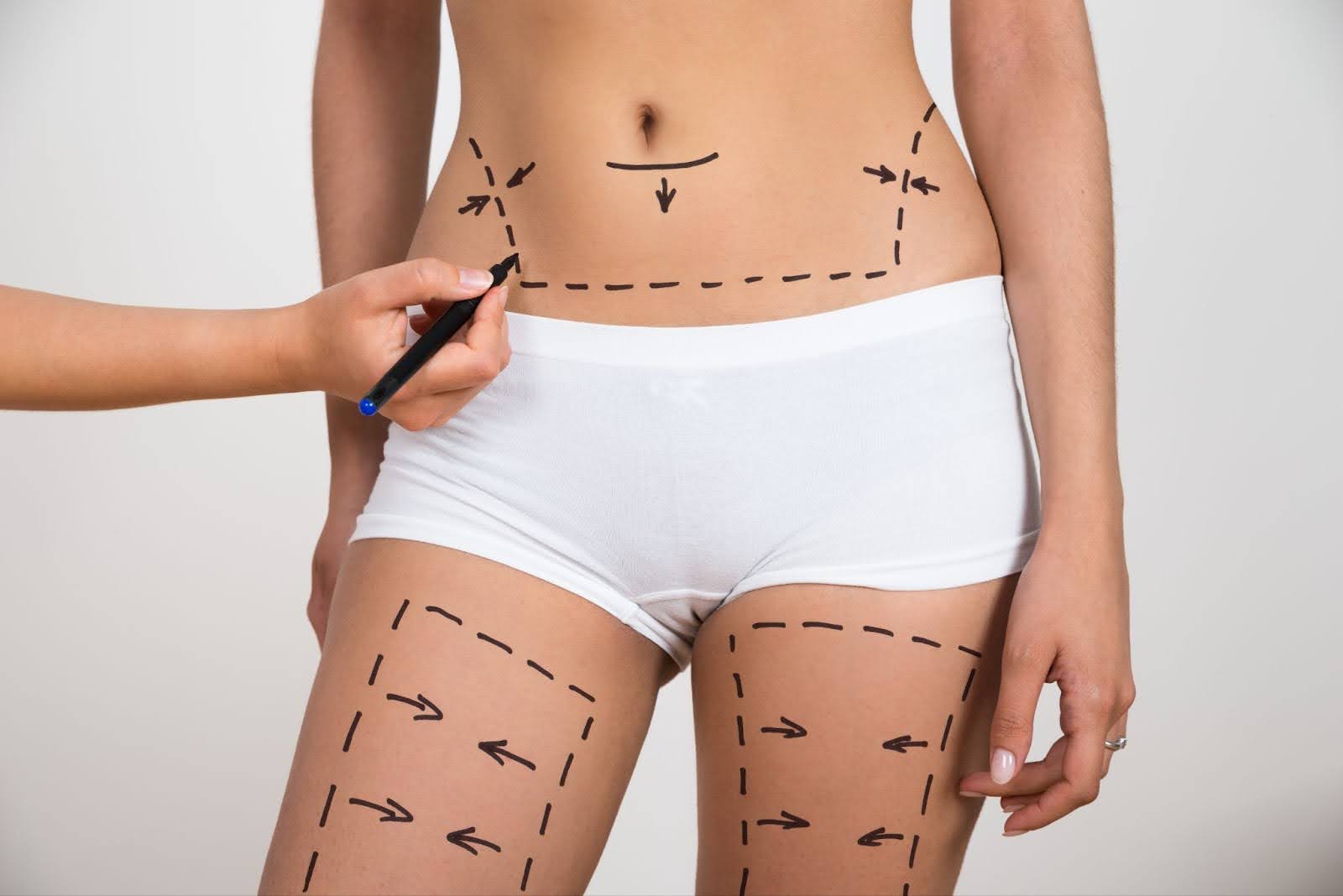
Source: shutterstock.com/ Photo Contributor: Andrey_Popov
Breast surgery
Breast augmentation
According to the Women’s Health and Cancer Rights Act of 1998 (WHCRA), all health insurance that covers mastectomies must also cover breast reconstruction. The law also allows women who undergo mastectomies to wait a few years to get breast augmentation.
Breast augmentation covered by insurance also extends to patients who have suffered a traumatic breast injury. Health insurance might cover the cost of reconstructive surgery, including implants, to achieve a symmetrical look.
Breast reduction
Women with large breast size often feel significant pain due to their weight. The breast size may also cause back problems, neck pain, shoulder grooving, and other complications.
Due to the issues and physical pain caused, the size interferes with the person’s quality of life. In this case, breast reduction surgery might be medically necessary to improve the quality of life and alleviate pain and other symptoms.
Gynecomastia
Some health plans may also cover gynecomastia or enlarged breasts in men. Gynecomastia may cause a lot of suffering in men, physically and mentally. Due to this, many insurance providers may provide provisions to cover breast reduction as a medical necessity.
If you seek gynecomastia, contact your medical insurance provider to check if they cover it. Sometimes, male breast cancer and gynecomastia are paired. This means that if malignancy is suspected, it will be a factor in determining how to proceed.
Butt lift
When you have a mastectomy and then a breast augmentation, your surgeon takes tissue from your buttocks area for breast reconstruction. Since the removal of skin is essentially a side effect of the mastectomy, your insurance provider is likely to cover a butt lift after the procedures.
Rhinoplasty (Nose job)
Insurance providers may cover a nose job (rhinoplasty) to possibly improve a patient’s ability to breathe properly. For example, your insurer will cover the repair if you have a deviated septum. Yet, if you also want to reshape your nose during the surgery, you may need to cover that cost yourself.
Also, if a patient has a narrow nasal passage obstructing their breathing, insurance might cover the surgery to resolve the issue. As a side benefit of the surgery, the patient may get a more appealing nose in shape, size, and contour.
Eyelid surgery (Blepharoplasty)
As we age, the upper eyelid skin starts to sag, which not only causes self-image issues but also hinders vision. If your vision is significantly impaired, your insurance provider may cover eyelid surgery (blepharoplasty).
In order to determine if a blepharoplasty will improve your vision, your primary care physician or plastic surgeon may order a visual field test.
Skin removal (Panniculectomy)
While some insurers may cover weight loss surgery, the procedures after are considered cosmetic and thus elective. However, in cases of extreme weight loss, skin removal plastic surgery may be medically necessary.
Panniculectomy is the removal of excess skin that causes pain and mobility issues for the patient. Due to the skin flaps causing pain, immobility, or infections, insurance providers may cover skin removal surgery. Alongside the panniculectomy, the insurance may cover abdominoplasty for the best results.
Botox
Many people immediately associate botox with aesthetic procedures when they hear it. Botulinum toxin might also be helpful for migraine treatment. For your insurance provider to cover botox for migraine, you may need to provide accurate documentation and medical history.
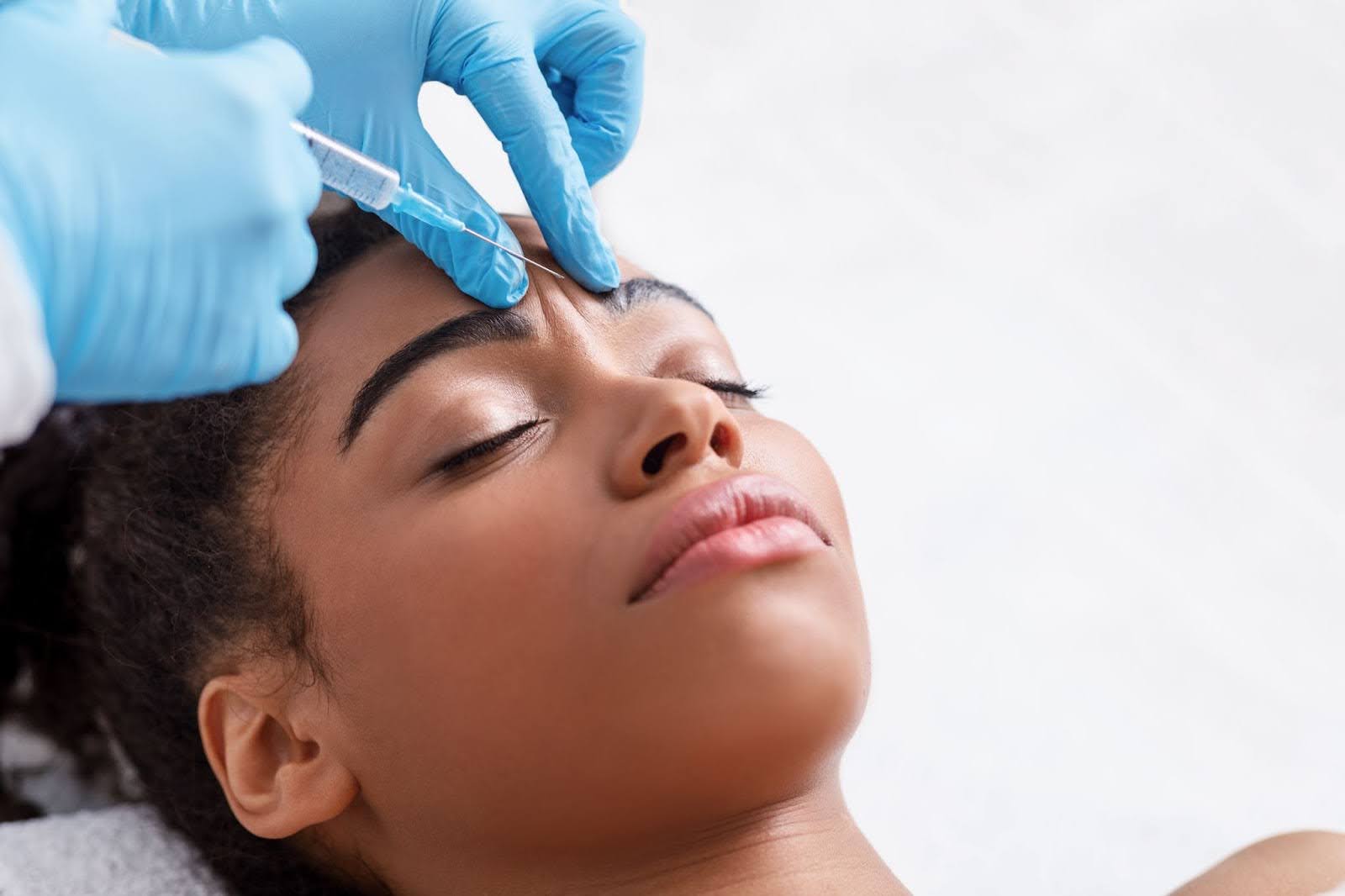
Source: shutterstock.com/ Photo Contributor: Andrey_Popov
How to Get Liposuction Covered by Insurance
Generally, liposuction is an elective surgery that insurance providers do not cover. The main purpose of liposuction is usually to improve the aesthetic appearance without any medical reasons.
That said, you may sometimes get your insurer to cover liposuction. There are two medical reasons insurers provide coverage for liposuction.
The first reason is obesity. If a person who is obese has their life quality impacted by it, medical insurance may cover liposuction. Another instance is the removal of a lipoma. A lipoma is a fatty tissue growing under the skin; it is removed with liposuction.
How to Get a Tummy Tuck Paid for by Insurance
Most often, a tummy tuck falls under the category of elective cosmetic surgery. Still, a tummy tuck may be deemed medically necessary and covered by health insurance. The following reasons are deemed medically necessary for a tummy tuck.
Correcting muscle separation
Several factors may lead to the separation of the abdominal wall muscles, including:
- Pregnancy
- Weight gain
- Aging
The separation of the abdominal muscle wall is known as diastasis recti. Diastasis recti happens when the six-pack ab muscles (rectus abdominis) separate due to being stretched.
The condition most often affects pregnant women. But as we mentioned, it can also be a byproduct of weight gain and aging.
Separation of abdominal muscles may cause back pain, digestive issues, and poor posture. In this case, a tummy tuck may be deemed medically necessary and covered by insurance to tighten the abdominal muscles.
Treating hernias
When patients develop hernias in their abdominal area, they may require surgical intervention. Surgeries on hernias are medically necessary. The surgeon may perform a tummy tuck during the procedure.
Getting Your Plastic Surgery Covered by Medical Insurance
The final decision lies with your insurance provider. Still, you may take some steps to strengthen your chances of getting insurance. Follow the steps to make the process easier:
- Compile all your condition and symptoms documentation, including photos and doctor visits.
- Provide proof of the methods and treatments you tried that have proven unsuccessful. This shows that plastic surgery is your last resort to fix the issue, as all other solutions have failed.
- Keep records of all the medications, hospital visits, sustained trauma, or other things regarding the condition.
- Ensure that you choose a board-certified surgeon with a great reputation. Having a reputable surgeon may increase the chances of the insurance provider to consider your case.
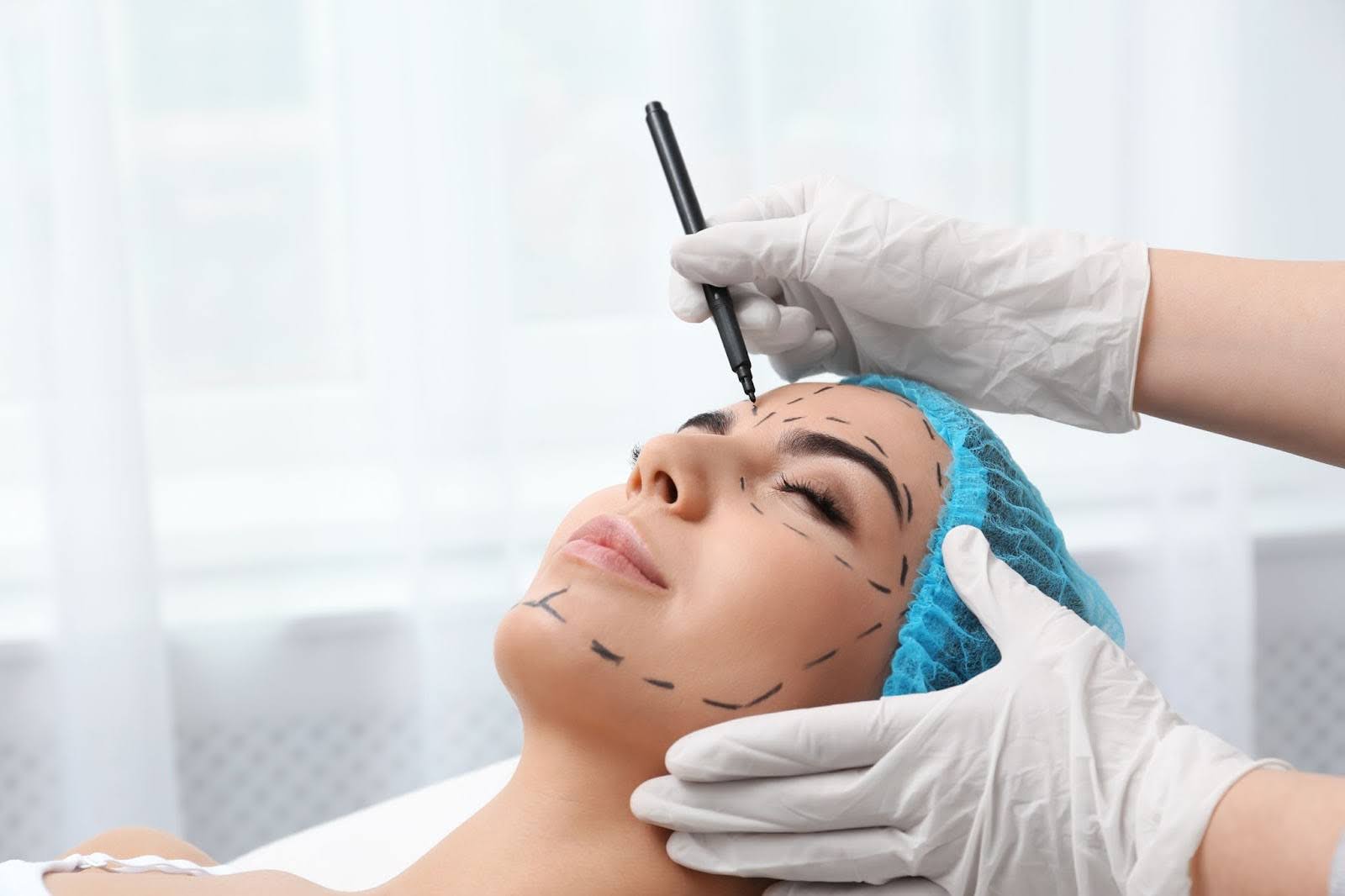
Source: shutterstock.com/ Photo Contributor: Andrey_Popov
Frequently Asked Questions
What is classified as cosmetic surgery?
Cosmetic surgery involves procedures that change the physical appearance for aesthetic rather than medical reasons. This is why they are elective; insurance providers usually do not cover their costs. However, there are exceptions if cosmetic surgery might relieve a medical condition.
What insurance covers plastic surgery?
Unlike cosmetic surgery, plastic surgery is reconstructive and medically necessary. This means insurance covers it. So, if you wonder, “What cosmetic surgery is covered by insurance?” the answer is as long as you can prove it has medical benefits.
